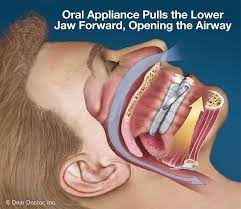
Sleep Apnea Treatment
Non-CPAP Sleep Apnea Treatment
At Sleep Solutions, we have a singular focus: to help you reclaim your sleep and, by extension, your health. We achieve this through two primary treatments: oral appliance therapy for sleep apnea and laser therapy for snoring. We believe that by offering only non-invasive, CPAP-free solutions, we can help individuals like you enjoy better sleep, improved health, and enhanced quality of life.
Oral Appliance Therapy
Oral Appliances for Sleep Apnea
Oral appliances are custom-fitted devices worn in the mouth during sleep. They resemble mouth guards used in sports. The primary function of these appliances is to maintain an open, unobstructed airway in the throat. They do this by repositioning the lower jaw, tongue, and soft palate. As a result, they reduce airway collapse and prevent interruptions in breathing during sleep.

Frequently Asked Questions About Sleep Apnea Treatment with Oral Appliances
1. How effective are oral appliances compared to CPAP machines?
Oral appliances are highly effective for many individuals, particularly those with mild-to-moderate OSA. While CPAP is considered the gold standard, oral appliances offer a more comfortable and portable alternative for some. They are best suited for patients who travel frequently or find CPAP machines cumbersome.
2. Are there any side effects of using oral appliances?
Most users adapt well to oral appliances. However, some may experience minor side effects like discomfort, excessive salivation, or changes in bite. These issues are usually temporary and can be managed with the help of a dental specialist.
3. Can oral appliances cure sleep apnea?
Oral appliances do not cure sleep apnea but effectively manage its symptoms. Regular use can significantly reduce apnea episodes, leading to better sleep quality and reduced health risks associated with OSA.
4. How do I know if an oral appliance is right for me?
Our dental sleep specialist, Dr. Perry, will evaluate your specific condition, considering the severity of your OSA and other factors, to determine if an oral appliance is suitable for you.
5. How long does it take to see results with an oral appliance?
Many users notice improvements within a few days. However, it’s important to have regular follow-ups with Dr. Perry to ensure the appliance is working effectively and to make any necessary adjustments.
Schedule a free consult today!
If you’re concerned you may have sleep apnea or snoring that affects your sleep, schedule a free consultation with us today. Dr. Perry is highly trained in sleep medicine and can help you start your journey to a good night’s sleep. Read on to learn more about sleep apnea.
Understanding Sleep Apnea: Symptoms, Causes, and Risk Factors
Sleep apnea (SA) is a common sleep disorder that causes frequent pauses in breathing during sleep. Most people with it experience symptoms such as loud snoring and daytime sleepiness. The two main types of SA are obstructive sleep apnea (OSA) and central sleep apnea (CSA), with treatment depending on the type. In OSA, a narrowing of the airway during sleep leads to breathing disruptions. A lack of communication between the brain and the breathing muscles in CSA is what causes the breathing disruptions. These breathing interruptions reduce the quality of sleep and, if left untreated, can lead to potentially serious health consequences, including erratic blood sugar levels. It’s critical to work with a doctor if you think you may be at risk for it so that you can get any necessary testing and treatment.
What is sleep apnea?
SA is a type of sleep-related breathing disorder, a group of sleep disorders characterized by abnormal breathing patterns during sleep. People with it repeatedly have reductions or pauses in breathing for brief periods while they sleep. Although these lapses cause a person to awaken periodically and reduce sleep quality, sleepers may not fully wake up and remain unaware that their nighttime breathing is abnormal. OSA in adults and central sleep apnea are two of the various types of it that can cause breathing interruptions.
Obstructive Sleep Apnea
OSA occurs when the airway at the back of the throat becomes constricted or blocked during sleep, which may cause snoring as air is prevented from passing through normally. A person typically awakens in response to an obstruction of the airway, contracts the muscles in their throat, and takes several deep breaths or gasps, frequently with sounds like snorting or choking. OSA is the most common type of it. It is estimated to affect 10% to 30% of adults in the United States, but in many cases, it goes undiagnosed.
Central Sleep Apnea
Central sleep apnea (CSA) involves disruption in the communication between the brain and the muscles that control breathing. As a result, breathing may become shallower and have temporary pauses, leading to drops in blood oxygen levels. The prevalence of CSA is low compared to obstructive sleep apnea. It is estimated that less than 1% of people have it.
Symptoms of Sleep Apnea
The symptoms include the effects of abnormal nighttime breathing as well as the daytime effects of reduced sleep quality.
Some common nighttime symptoms include:
1. Loud, persistent snoring
2. Long pauses in breathing during sleep
3. Gasping or choking noises during sleep
4. Restless sleep
5. Waking up frequently during the night
Daytime symptoms of SA can include:
1. Excessive daytime fatigue or sleepiness
2. Morning headaches
3. Difficulty concentrating
4. Irritability or mood changes
5. Dry mouth or sore throat upon waking
6. Decreased libido or sexual dysfunction, which people with SA might experience
If left untreated, SA can lead to more serious health issues such as hypertension, heart disease, stroke, and diabetes. It is important to seek medical evaluation and treatment if you suspect you may have it.
Symptoms of Obstructive Sleep Apnea
Frequent symptoms include:
- Excessive daytime sleepiness, often a symptom of SA, increases your risk for day-to-day functioning issues., which can signal sleep apnea or another serious sleep disorder.
- Loud snoring that frequently includes gasping or choking sounds
- Headaches in the morning that may persist for several hours after waking up
- Dry mouth upon awakening, which can be a symptom of sleep apnea, particularly if the individual uses a CPAP machine.
- Restless sleep with periods of wakefulness during the night is a hallmark of both mild sleep apnea and more severe forms, impacting blood oxygen levels and overall health.
- Increased need to get up from bed to urinate, a symptom that people with sleep apnea might notice.
- Irritability or frustration
- Reduced focus can sometimes be an indicator of severe sleep apnea.
Certain symptoms of obstructive sleep apnea may not be immediately noticeable but can significantly impact quality of life, prompting a doctor to refer you to a sleep center for further evaluation. to the person with the condition. For instance, a person might not notice their snoring and abnormal breathing until their bed partner does. The complexity of symptoms and causes of obstructive sleep apnea makes it difficult to diagnose the condition, including treatment-emergent central sleep apnea, by symptoms alone.
Symptoms of Central Sleep Apnea
The symptoms that are most often associated with central sleep apnea include:
- Abnormal breathing patterns, such as breathing that slows down, speeds up, and pauses during sleep
- Excessive daytime sleepiness
- Nighttime awakenings often occur in individuals with mild sleep apnea.
- Sudden shortness of breath or chest pains at night are potentially indicative of sleep apnea episodes causing sudden drops in blood oxygen.
- Difficulty focusing
Blood oxygen levels can also have an impact on morning headaches, a common symptom of SA. As with OSA, it is typical for people with CSA to be unaware of their irregular breathing during sleep unless a bed partner or caregiver points it out.
Causes of Sleep Apnea
The cause of breathing disruptions differs between OSA and CSA. Usually, a physical obstruction of the airway, such as relaxed throat muscles or extra tissue blocking the airway, is what causes OSA. This obstruction leads to pauses in breathing during sleep as the individual struggles to take in enough oxygen. On the other hand, central sleep apnea, also known as CSA, is a condition that results from a problem with the brain’s ability to control breathing. The brain fails to send the proper signals to the muscles that control breathing, resulting in reduced or paused breathing during sleep. CSA is often linked to underlying medical conditions such as heart failure, stroke, or brainstem injury.
Causes of Obstructive Sleep Apnea
In people with OSA, the muscles in the back of the throat relax during sleep, reducing space for air to pass through. Snoring occurs as the airway narrows, and when the airway is obstructed, a person fails to get enough oxygen. The lack of oxygen causes partial or complete awakenings in order to restore airflow. These breathing disruptions, characteristic of SA, happen repeatedly during sleep.
Causes of Central Sleep Apnea
CSA arises because of problems in how the brain communicates with the muscles responsible for breathing. For people with CSA, a part of the brain called the brain stem fails to properly recognize carbon dioxide levels in the body during sleep, which underscores the symptoms and causes of this form of SA. This leads to repeated episodes of breathing that are slower and shallower than it should be.
Risk Factors for Sleep Apnea
Multiple factors affect a person’s chances of developing sleep apnea, and those factors are different for OSA and CSA.
For obstructive sleep apnea (OSA), risk factors include conditions that increase sleep apnea risk:
1. Obesity: Excess weight can lead to the narrowing of the airway, making it more difficult to breathe during sleep.
2. Age: OSA is more common in older adults, indicating that sleep apnea usually becomes more prevalent with aging.
3. Gender: Men are at higher risk of developing OSA than women. Complex sleep apnea, where obstructive sleep apnea is combined with central sleep apnea, is less common but severely impacts sleep quality. Family history: OSA can run in families, suggesting a genetic component.
4. Smoking: Smoking can increase inflammation and fluid retention in the upper airway, contributing to OSA.
5. Alcohol and sedative use: These substances relax the muscles in the throat, increasing the risk of airway blockage during sleep and elevating sleep apnea risk.
For central sleep apnea (CSA), risk factors include:
1. Heart disorders: Conditions such as congestive heart failure, atrial fibrillation, and stroke can disrupt the brain’s signaling to the respiratory muscles, leading to CSA.
2. Age: CSA is more common in older adults.
3. Opioid use: Certain medications, such as opioids, can affect the brain’s control of breathing, leading to CSA.
4. Neurological disorders: Conditions such as Parkinson’s disease, ALS, and stroke can affect the brain’s ability to regulate breathing, increasing the risk of CSA.
It is important to note that these risk factors are not definitive predictors of SA, and a person may develop the condition even without these factors present. Additionally, lifestyle changes and treatment options are available to manage and improve symptoms of SA, regardless of the underlying risk factors.
Risk Factors for Obstructive Sleep Apnea
The primary risk factors for obstructive sleep apnea are related to age, sex, body weight, and certain anatomical features of the head and neck area.
- Age: The risk of developing obstructive sleep apnea increases with age until a person is in their 60s and 70s, indicating that sleep apnea usually becomes more common as people age.
- Sex: Men or people assigned male at birth are generally more likely to have obstructive sleep apnea, especially in the earlier stages of adulthood, highlighting the demographic trends in obstructive sleep apnea in adults.
- Head and neck anatomy: Obstructive sleep apnea occurs more frequently in people who have specific anatomical features, including a larger tongue and a shorter lower jaw.
- Body weight: Multiple studies have found a correlation between a higher body mass index (BMI) and an elevated risk of developing obstructive sleep apnea, as excessive weight increases your risk for this condition.
- Cigarette smoking: Some research has found a noticeably higher risk of obstructive sleep apnea in people who smoke cigarettes compared to those who have quit or never smoked, indicating smoking as a factor that increases sleep apnea risk.
- Hormone abnormalities: Hormone conditions like an underactive thyroid or excess production of growth hormone may increase the risk of OSA by causing swelling of tissue near the airway or by contributing to a higher body mass index.
- Sleeping position: Sleep apnea may develop or worsen when people sleep on their backs because of how that sleeping position affects the shape and positioning of the tissue around the airway.
- Family history of sleep apnea: There are some indications that a family history of OSA can increase a person’s risk of obstructive sleep apnea, which may relate to anatomical features in the head and neck that are shared among family members.
- Nasal congestion: Difficulty breathing through the nose has been linked with a higher likelihood of having OSA.
- Using alcohol and some medications: Alcohol and some prescription and narcotic drugs are associated with an elevated risk of obstructive sleep apnea.
- Certain medical conditions: People with some medical problems, including several heart and lung conditions, may have a greater tendency to develop OSA.
Risk factors for central sleep apnea also include variables that may exacerbate the condition, similar to obstructive sleep apnea, which happens in adults and requires personalized approaches to treatment for sleep apnea. Central sleep apnea most often occurs as a consequence of another medical problem, such as an infection or injury affecting the brain stem. Conditions like heart or kidney failure, stroke, or excess growth hormone production can exacerbate sleep apnea by affecting blood oxygen levels during sleep. Studies have identified some additional factors that are linked to a heightened risk of central sleep apnea.
- Age: People who are over 65 have a heightened risk of breathing disruptions consistent with central sleep apnea.
- Sex: Central sleep apnea is more common in men or people assigned male at birth, which may be related to levels of certain sex hormones.
- Use of certain drugs: Chronic use of opioid drugs and some prescription medications can affect breathing and have been associated with a higher risk of CSA.
- Being at high altitude: Spending time at high altitude is associated with CSA because of the decreased availability of oxygen in high-altitude environments.
How is sleep apnea diagnosed?
A doctor or sleep specialist in sleep medicine must diagnose sleep apnea, and there are several steps in the diagnostic process, including an evaluation of blood oxygen levels and sleep patterns. The first step in diagnosing sleep apnea is usually a comprehensive evaluation of the patient’s symptoms and medical history, focusing particularly on sleep apnea risk factors. This may involve questions about the patient’s sleep habits, daytime symptoms such as excessive daytime sleepiness or fatigue, and any other relevant medical conditions. After the initial evaluation, the doctor may recommend a sleep study, also known as a polysomnogram, to confirm the diagnosis of sleep apnea. During a sleep study, the patient spends the night in a sleep lab or may do a home sleep study where they wear a device that monitors their breathing, heart rate, oxygen levels, and other factors while they sleep.
In addition to the sleep study, the doctor may also order other tests, such as a blood test, to check for underlying conditions, such as thyroid problems, that may be contributing to the sleep apnea. Once the diagnosis of sleep apnea is confirmed, the doctor will work with the patient to develop a treatment plan. This may involve lifestyle changes such as weight loss or quitting smoking, using a continuous positive airway pressure (CPAP) machine while sleeping, or, in some cases, surgery to correct anatomical issues that may be causing the apnea. Overall, the process of diagnosing sleep apnea is crucial in order to effectively manage the condition and improve the patient’s overall health and quality of life.
Health History and Physical Exam
An evaluation for sleep apnea typically starts with a review of a person’s symptoms and overall health, as well as a physical exam. This is designed to detect signs of sleep apnea and identify risk factors that could contribute to the condition. Although testing is required to confirm that someone has OSA, the presence of symptoms can factor into the diagnosis and help determine the severity of the condition.
Sleep Study
A sleep study is necessary to diagnose obstructive or central sleep apnea. The most dependable kind of sleep study is called polysomnography, which is conducted during an overnight stay at a specialized sleep laboratory to accurately diagnose and treat sleep apnea. During polysomnography, multiple sensors are used to track breathing, awakenings, oxygen levels, muscle movement, sleep stages, and other aspects of sleep. An in-clinic sleep study can determine if breathing is abnormal and differentiate between obstructive and central sleep apnea. For OSA, polysomnography may involve either one or two visits to a sleep clinic. An at-home sleep study for obstructive sleep apnea is an option for certain patients who are believed to have more severe OSA. Although taking a sleep apnea test at home may be more convenient, a health professional must still interpret the results. Home testing is not used for central sleep apnea.
Treatments for Sleep Apnea
The goal of treatment for SA is to reduce breathing disruptions and improve sleep. The approach to treatment varies between OSA and CSA. For OSA, the primary treatment option is continuous positive airway pressure (CPAP) therapy, a method to ease your symptoms. This involves wearing a mask over the nose and/or mouth during sleep, which delivers a continuous flow of air to keep the airway open. Other treatment options for OSA include oral appliances that help keep the airway open, non-invasive laser treatment to regenerate collagen at the back of the throat and open the airway more, surgery to remove excess tissue in the throat, or weight loss in cases where obesity is a contributing factor.
CSA is often treated with positive airway pressure therapy as well, but may also require additional treatments such as medications to stabilize breathing patterns or treating underlying medical conditions that may be causing the CSA. In some cases, a combination of treatments may be necessary to effectively manage sleep apnea and improve symptoms. It is important for individuals with SA to work closely with their healthcare provider to find the most appropriate treatment plan for their specific needs. Additionally, making lifestyle changes such as maintaining a healthy weight, quitting smoking, and avoiding alcohol and sedatives before bed can also help improve SA symptoms.
Treatments for Obstructive Sleep Apnea
Positive airway pressure (PAP) therapy is a treatment offered to almost all people with OSA. PAP therapy keeps the airway open with pressurized air that is pumped from a machine through a hose and a mask worn on the face. PAP devices, a type of positive airway pressure device, are only available with a prescription for people with sleep apnea. Their air pressure must be carefully calibrated in a process called titration that occurs during a sleep study to effectively treat SA.
A common type of PAP therapy uses a continuous positive airway pressure (CPAP) device that sends a stream of air that is always set to the same pressure level. Other types of PAP devices, such as bi-level positive airway pressure (BiPAP) and auto-titrating positive airway pressure (APAP), provide variability in the amount of air pressure. Some types of mouthpieces that hold the jaw or tongue in a specific position are a treatment option for people with certain anatomical features and less severe OSA. People who experience difficulties or discomfort using PAP devices may prefer these oral appliances, which can reduce snoring but frequently do not improve breathing as much as PAP therapy. Surgery to remove tissue in the throat and expand the airway can be a treatment option for patients who have tissue obstructing their airway. Another type of surgical treatment requires implanting a device to stimulate a nerve that helps control breathing. Laser therapy for SA is a non-invasive procedure that rebuilds collagen at the back of the throat, opening up the airway.
An additional component of treatment for obstructive sleep apnea involves lifestyle changes to help manage symptoms. These suggestions may include:
- Reducing BMI by losing weight
- Getting regular exercise, which may decrease OSA symptoms even without weight loss,
- Altering sleeping position to avoid back sleeping can be an easy treatment strategy for some individuals with mild SA.
- Reducing alcohol consumption
Treatments for Central Sleep Apnea
Treatment for CSA often focuses on addressing the medical issue causing abnormal breathing. If sleep disruptions are mild, treatment for the underlying cause may be all that is required. However, if the symptoms of CSA are persistent or severe, additional treatment may be recommended to improve breathing while also trying to resolve the underlying problem. This may include the use of PAP devices to promote steadier breathing during sleep. Other possible treatments include supplemental oxygen therapy or the use of medication that can speed up a person’s breathing. The complications of SA can severely impact health, including blood sugar levels. Effective treatment can generally prevent or resolve serious complications from SA, but if the condition is left untreated, it can have far-reaching effects on health and well-being. SA lowers sleep quality, and because it has an impact on the body’s oxygen levels, it exacerbates the effects of poor sleep.
Accordingly, OSA has been associated with a higher risk of a diverse range of health problems, including:
- Car accidents from drowsy driving
- Cardiovascular diseases like high blood pressure, stroke, heart failure, heart disease, and an abnormal heartbeat
- Metabolic disorders, including type 2 diabetes
- Pulmonary hypertension, which is high blood pressure in the arteries of the lungs that places an excess strain on the heart,
- Thinking problems such as impaired memory and concentration
- Mood disturbances, including irritability and a higher risk of depression
- Nonalcoholic fatty liver disease, which is an increase in fat deposits in the liver that can contribute to serious liver damage, especially in patients with sleep apnea without adequate treatment,
- Anesthesia-related complications during surgery
In CSA, the complications that can occur depend largely on the underlying medical issue causing breathing to be disordered.
Sleep Apnea in Children
Although frequently associated with older adults, SA can occur in children. In young people, OSA is much more common than central sleep apnea. It is estimated that 1% to 5% of children have it. Children with OSA may not experience excessive daytime sleepiness as seen in adults with sleep apnea. Instead, they may exhibit daytime symptoms like hyperactivity, learning difficulties, or behavior problems. As in adults, snoring is common for children with obstructive sleep apnea. However, children may have other nighttime symptoms like sweating, bedwetting, or sleepwalking. Children with severe, untreated OSA may also experience problems with their growth and development. Large tonsils and adenoids in the throat are a common cause of obstructive sleep apnea in children, and surgery to remove these tissues may be an option for treatment.
Living with Sleep Apnea
Practical steps can help people living with SA cope with this condition and its potential health effects. Work closely with a doctor: It is important to stay in touch with a primary care doctor, a specially trained dentist, or a sleep specialist and report any ongoing symptoms, challenges with treatment, or other concerns that may require an adjustment to the plan for managing it.
- Properly care for treatment devices: Whether using a PAP device or an oral appliance, cleaning and maintenance can help get the most out of treatment and avoid unwanted side effects.
- Avoid high-risk activities: People with SA should be aware of the risks of daytime sleepiness. Especially for people with untreated sleep apnea, activities like driving or operating heavy machinery should be avoided when drowsy.
- Consider changing sleeping positions. Although they have not been rigorously studied, special products to avoid back sleeping may help some people reduce their symptoms of OSA.
- Minimize alcohol consumption: Reducing alcohol intake can be a component of the treatment plan for sleep apnea, as alcohol increases your risk of breathing disruptions during sleep. In people with untreated OSA, even daytime alcohol consumption may exacerbate breathing problems at night.
- Inform new doctors about sleep apnea: People with sleep apnea should mention this condition to any new medical providers, especially when planning to start a new medication or undergo surgery, as it may impact their sleep medicine regimen.
Download The SnoreLab App
We highly recommend downloading this app and recording the audio of a couple of nights of sleep. The app comes with a free week trial. Make sure you cancel the trial before it ends so you’re not charged. Take screenshots of your results and bring them to your consultation with us.
Don't let sleep apnea and snoring hold you back from the life you deserve.
Choose Sleep Solutions, where we turn every night into a step toward better health.